Provocative Mesenteric Angiography (PMA) to Treat Lower GI Bleeding
Provocative mesenteric angiography or PMA, is an ill-researched method to treat gastrointestinal bleeding. LAIIC's interventional radiology team contributed to groundbreaking new research about PMA, which was published in the August edition of the Journal of Gastrointestinal Surgery.
Why is provocative angiography research important?
The role of provocative mesenteric angiography is to potentially provide a better method to treat gastrointestinal bleeding. The outcomes of colonoscopy via traditional angiography is subject to variable outcomes due to fear of hemorrhagic complications.
LAIIC's Dr. Sabeen Dhand contributed to the provocative angiography research which spanned a 12-year review period and 36 PMAs.
What were the results of the mesenteric angiography study?
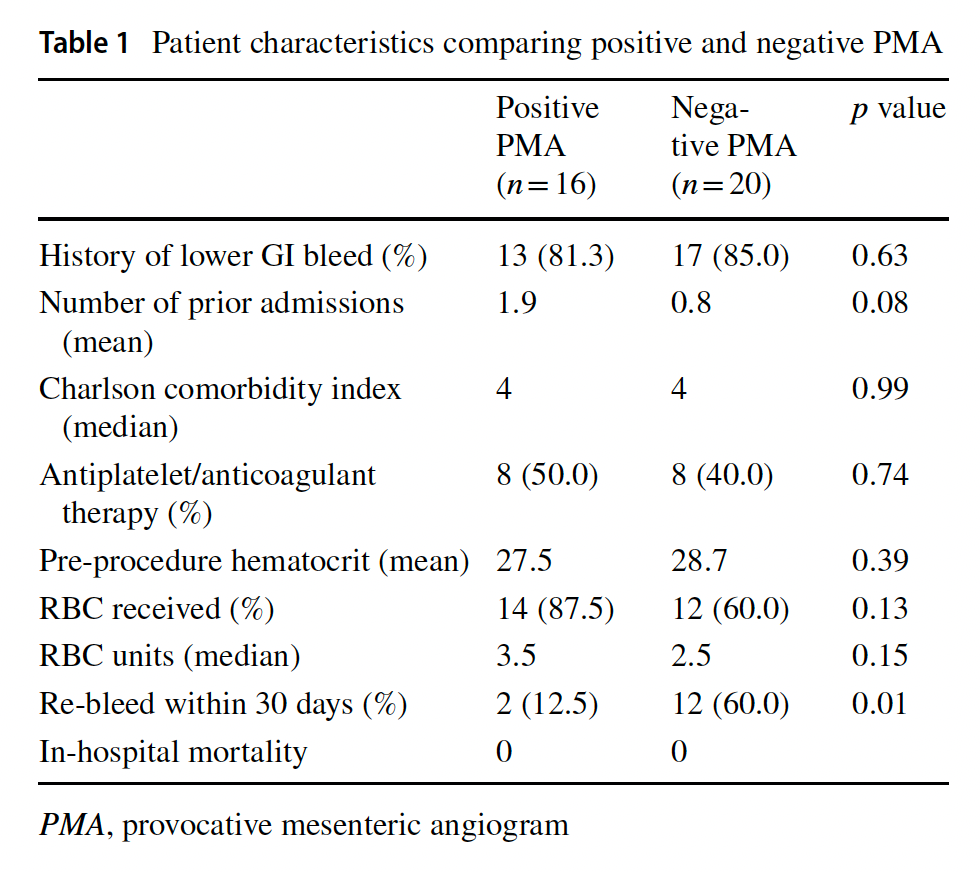
The mesenteric angiography research study showed that patients positive for PMA saw significantly fewer cases of recurrent bleeding within 30 days! Of the 16 positive PMA cases reviewed, only 2 of 16 cases (or 12.5%) saw recurrent bleeding within 30 days versus the 12 of 20 cases (or 60%) who were negative for PMA and saw recurrent bleeding within 30 days after the procedure.
The angiography study saw no significant difference between patients admitted to the study along the following dimensions:
- Demographics
- Previous history of lower GI bleeding
- Number of prior admissions
- Patient morbidity by Charlson comorbidity index
- Pre-procedure hematocrit
Of note, no major or minor complications occurred in patients undergoing the PMA procedure.
Other takeaways from the angiography study
This is the largest provocative angiography study of its kind in history, and LAIIC's interventional radiology team is honored to have been a contributor. Alongside the other radiology teams, they found the following takeaways:
- Provocative angiography allowed for the positive identification of lower GI bleeding in 44% of cases that were initially deemed negative for the condition.
- This allowed for embolization in 100% of those cases, in which significantly fewer patients readmitted relative to those negative for PMA (12.5% vs. 60%).
- The 50mg maximum dose of tPA used in the study is greater than that used in most PMA studies, which suggests that the higher dose can be safely administered without adverse effects.
In conclusion, the provocative mesenteric angiography procedure was found to be safe in this study with no bleeding or ischemic bowel complications–even at the higher tPA dose.
The proposed protocol for incorporating PMA in patients with lower GI bleeding can be found in the below diagram:
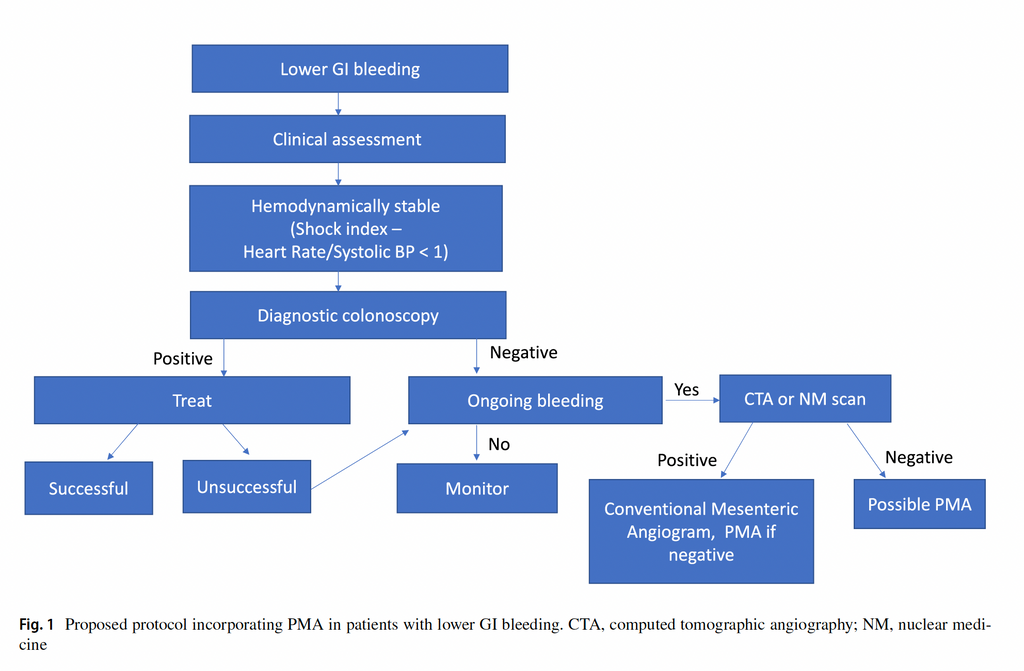
The study is subject to inherent single-institution bias, and may not be typical for some patients diagnosed at outside institutions with different medical charting in the follow up. To preview the study in its entirety, please view it here.
Have any questions about this procedure to treat lower gastrointestinal bleeding? Contact our radiology team here.

